What is Nutrition Medicine?
Many of the health challenges faced by a growing number of people today are complex and have multiple components. This means that simple diagnoses and appropriate treatments are not provided by conventional medicine. A large number of people are left frustrated as there appears to be no identifiable medical cause and therefore no solutions offered. In the field of nutrition/functional medicine, the goal is to work adjunct to conventional medicine to identify the root cause of the health issues by assessing multiple body systems in an integrated way and to identify triggers and accelerators that perpetuate the condition.
The world has benefited from great successes in treating disease, but also created new health problems due to practices introduced for food production and processing in addition to unprecedented levels of toxin exposure. This means that more holistic, integrated approaches that consider the interconnection of our biochemistry and metabolism with the environment are required to help understand and treat the basis of modern multifactorial health conditions.
The human body is remarkable as it has the capacity to adapt to a changing environment and heal itself, provided it is allowed to express it genetic potential. It does this only if it is provided with the raw materials for healthy metabolic function:

So why Nutrition Medicine?
Nutrition may the most influential component in maintaining health but we know this as many modern chronic diseases are diet related, including heart disease, diabetes, obesity, liver disease and cancer. Yet the problem lies in determining what is optimal nutrition for each person as this is highly variable between different people. Why are some diets suited to some and not others? We need to think in terms of personalised medicine and individual nutritional requirements.
Biochemical individuality influences not only an individual’s requirement for various nutrients but also what the signs and symptoms of any nutrient insufficiency will be. This makes the recommended dietary intake (RDI) levels for many nutrients quite useless.  These are most useful for establishing the minimum amounts of a nutrient that your body requires on a daily basis before you start to show signs of a frank deficiency of a nutrient such as seen in pellagra, beriberi and scurvy. These are taught as single nutrient deficiency diseases characterised by a specific set of symptoms which progress in a predictable manner. However, it turns out not to be the case and the following excerpt is from a Chaplain’s account aboard HMS Centurion, highlighting how the concept of biochemical individuality is relevant even in a single nutrient deficiency disease and was clearly apparent centuries ago.
These are most useful for establishing the minimum amounts of a nutrient that your body requires on a daily basis before you start to show signs of a frank deficiency of a nutrient such as seen in pellagra, beriberi and scurvy. These are taught as single nutrient deficiency diseases characterised by a specific set of symptoms which progress in a predictable manner. However, it turns out not to be the case and the following excerpt is from a Chaplain’s account aboard HMS Centurion, highlighting how the concept of biochemical individuality is relevant even in a single nutrient deficiency disease and was clearly apparent centuries ago.
“This disease, so frequently attending all long voyages, and so particularly destructive to us, is surely the most singular and unaccountable of any that affects the human body. For its symptoms are inconstant and innumerable, and its progress and effects extremely irregular: for scarcely two persons have the same complaints, and where there is found some conformity in symptoms, the order of their appearance has been totally different. However though, it frequently puts on the form of many other diseases, and is therefore not to be described by any exclusive and infallible criterions”
~Chaplain Richard Walter, Anson’s Voyages Around the World in the Years 1740-1744.
626 of 961 men died of scurvy
Due to the fundamental role in cellular metabolism, even sub-optimal levels of essential nutrients can have system wide effects which can be further compromised by an individual’s biochemical expression determined by their genetics.
The practice of nutrition medicine is perfectly placed to investigate and help treat many of the conditions that conventional medicine may only have some answers for. While individual isolated symptoms may improve by targeted therapies, the questions of why the symptoms/condition developed in the first place largely remain unanswered.
So the typical patients we see often include:
- Fatigue
- Chronic pain
- Gut problems and food sensitivities
- Inability to lose weight
- Hormone imbalances
- Mood disorders
- Skin problems
- Elevated cholesterol
- Elevated blood pressure
- Metabolic syndrome
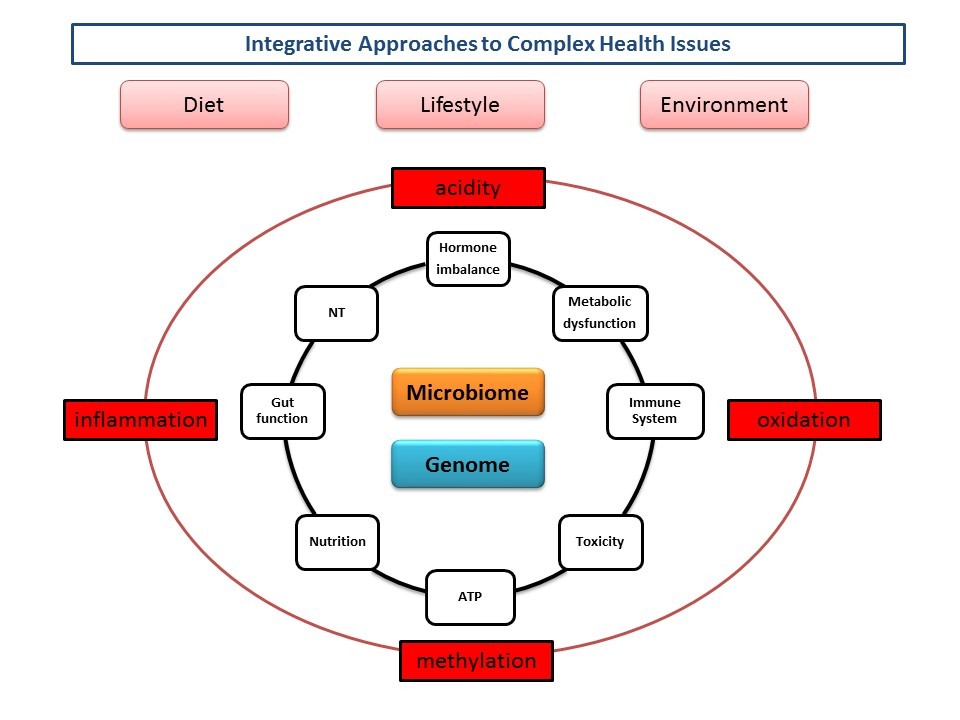
But rather than treat each of these ‘conditions’ as single isolated entities, we need to understand that each of those listed are likely to have overlapping components, which is described by the following schematic and illustrates the interaction between the diet, lifestyle and environment with our genetics and microbiome which ultimately influences multiple body systems and cellular function.

If you want to know more about nutrition medicine and how it can help you, don’t delay and book in to discuss it with the doctor at Cellf today.
Next blog will discuss genetic profiling and how a simple test can identify our biochemical vulnerabilities to enable targeted approaches to treatment.